Total Knee Replacement
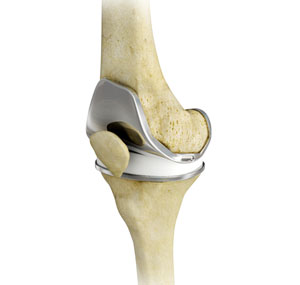
Total knee replacement, also called total knee arthroplasty, is a surgical procedure in which the worn out or damaged surfaces of the knee joint are removed and replaced with artificial parts. Arthritis (inflammation of the joints), injury, or other diseases of the joint can damage this protective layer of cartilage, causing extreme pain and difficulty in performing daily activities.
Am I a candidate for a knee replacement?
Total knee replacement surgery is commonly indicated for severe osteoarthritis of the knee. Osteoarthritis is the most common form of knee arthritis in which the joint cartilage gradually wears away. It often affects older people.
In a normal joint, articular cartilage allows for smooth movement within the joint, whereas in an arthritic knee the cartilage itself becomes thinner or completely absent. In addition, the bones become thicker around the edges of the joint and may form bony “spurs”. These factors can cause pain and restricted range of motion in the joint.
Your doctor may advise total knee replacement if you have:
- Severe knee pain which limits your daily activities (such as walking, getting up from a chair or climbing stairs).
- Moderate to severe pain that occurs during rest or awakens you at night.
- Chronic knee inflammation and swelling that is not relieved with rest or medications
- Failure to obtain pain relief from medications, injections, physical therapy, or other conservative treatments.
What are the causes of knee osteoarthritis?
The exact cause of osteoarthritis is not known, however there are several factors that are commonly associated with the onset of arthritis and may include:
- Injury or trauma to the joint
- Fractures at the knee joint
- Increased body weight
- Repetitive overuse
- Joint infection
- Inflammation of the joint
Do I need a knee replacement?
The first step when making the decision about knee replacement is to meet with your surgeon to see if you are a candidate for total knee replacement surgery. Your surgeon will take your medical history, perform a physical examination, and X-ray your knee. Even if the pain is significant, and the X-rays show advanced arthritis of the joint, the first line of treatment is nearly always non-operative. This includes weight loss if appropriate, an exercise regimen, medication, injections, or bracing. If the symptoms persist despite these measures, then you could consider surgery.
The decision to move forward with surgery is not always straight forward and usually involves a thoughtful conversation with yourself, your loved ones, and ultimately your surgeon. The final decision rests on you based on the pain and disability from the arthritis influencing your quality of life and daily activities. Those who decide to proceed with surgery commonly report that their symptoms keep them from participating in activities that are important to them (like walking, taking stairs, working, sleeping, etc.), and that non-operative treatments have failed.
How long will it last?
A common reply to this question is that total joint replacement lasts 15-20 years. A more accurate way to think about longevity is via the annual failure rates. Most current data suggests that both hip and knee replacements have an annual failure rate between 0.5-1.0%. This means that if you have your total joint replaced today, you have a 90-95% chance that your joint will last 10 years, and a 80-85% that it will last 20 years. With improvements in technology, these numbers may improve.
What types of implants will I get?
The orthopaedic implant industry has developed a number of innovative technologies in an effort to improve the outcomes of total joint replacement surgery. In recent years, these technologies have been marketed directly to patients, which has increased the awareness as well as confusion on what these different designs mean. The most important message is that while a certain manufacturer may claim that their design is better, almost all of the available registry data (large collections of data that track total joint surgery outcomes) show that there is no clear advantage to any of these designs when it comes to improving outcomes. Here are specific implant design terms:
- Gender specific: This refers to a modified implant design that accounts for average anatomic differences between men’s and women’s knees. Most manufacturers have incorporated similar modifications in their newer designs, which allow for more sizing options so that the prosthesis can be more accurately fit to the patient’s native anatomy and recreate the natural function of the knee.
- Rotating platform: This refers to a plastic bearing that independently rotates on a metal tray on which it is seated. More often, the plastic bearing locks into the metal tray – referred to as a “fixed bearing.” Some theoretical advantages to the rotating platform concept when it was initially designed was that it could reduce the wear of the plastic bearing, reduce the rate of loosening of the metal parts, and better replicate how a patient’s knee works (kinematics). Most current data shows that after five to ten years in use, there does not appear to be any difference between rotating platform and fixed bearing designs in any of these outcomes.
Will my surgeon use a computer, robot, or custom cutting guide in my surgery?
There are many studies attempting to evaluate these emerging technologies and their influence of the success of surgeries. Each of these technologies has a specific goal that has fueled its development (i.e. more accuracy in implant placement, more efficient or faster surgery, etc.).
To date, there appears to be both pros and cons to each of these technologies without any clear advantages, but more research is required to determine what advantage, if any, these may offer.
Despite a substantial amount of direct-to-consumer marketing, the best approach is to discuss this topic with your surgeon. You may want to know if they use one of these technologies, why they have chosen to do so, and what their experience has been in using it.
Currently th most significant factor for the patient’s outcome remains that any operation is performed by a skilled orthopaedic surgeon, whatever technology may or may not be used.
Is knee surgery and recovery very painful?
Pain following total knee replacement has come a long way over the last 10-15 years with increased use of regional nerve blocks, spinal blocks, and various other modalities used for pain control. Total hip replacement is generally considered to be less painful than total knee replacement. Early range of motion and rapid rehabilitation protocols are also designed to reduce early stiffness and pain, making the procedure in general much less painful than in years past. You may have relatively mild pain following the procedure, or you may have a more difficult time than others. Everyone is unique and handles and perceives pain differently. Currently we use patient education, multimodal pain strategies and the services of the acute pain service to maximise pain control both in hospital and during your rehabilitation. These advancements in anesthesia and pain management during and after total knee replacement surgery. All of these practices allow you to feel better, have less pain, and regain function faster than in the recent past.
How big will my scar be?
The size of the incision can vary and depends on several factors that include the size of the patient and the complexity of the surgery. Most studies have shown that smaller incisions offer no improvement in pain or recovery and may actually worsen the surgeon’s ability to adequately perform the procedure.
Can I get both knees replaced at the same time (a bilateral total knee replacement)?Both knees may be replaced under the same anaesthetic in certain cases. It is obviously a larger and longer procedure than a single knee replacement and the recovery is more difficult and prolonged. However for patients aged 70 or younger with symptomatic bilateral disease and are relatively fit and healthy (ASA status 1-2), this may be an option.
Will I need general anesthesia?
While general anesthesia is a safe option, knee replacements can be performed under regional anesthesia. Choices for regional anesthesia include spinal anesthesia, epidural anesthesia, or one of a variety of peripheral nerve blocks. Many surgeons and anesthetists prefer regional anesthesia because data shows it can reduce complications and improve your recovery experience with less pain, less nausea and less narcotic medicine required.
Recently, peripheral nerve blocks have become more popular as an adjunct for pain control. For total knee replacement this can include an adductor canal block, which allows pain control without causing weakness of your muscles. You should have a discussion regarding anesthesia and post-operative pain management with your surgeon and anesthesia team prior to your surgery.
How long will I stay in the hospital?
You will likely stay in the hospital for three to five days depending on your rehabilitation protocol and how fast you progress with physical therapy. This is highly dependent upon your condition before surgery, your age, and medical problems which can influence your rehabilitation. A safe discharge plan either home or to a rehabilitation facility will be arranged for you by the orthopaedic team.
How long does it take to recover?
It can take up to three months for you to return to most activities, and likely six months to one year to fully recover to maximal strength and endurance following total knee replacement surgery. This depends on your condition before surgery, additional medical problems, and your expectations.
Post-operative care
Rehabilitation begins immediately following the surgery. A physiotherapist will teach you specific exercises to strengthen your leg and restore knee movement. You will be able to walk with crutches or a walker. Your physiotherapist will also provide you with a home exercise program to strengthen thigh and calf muscles.
When can I shower?
Many surgeons use waterproof dressings that allow for showering as early as the day after surgery. It is usually recommended for no soaking the wound in a bath or a pool for three weeks to allow the incision to fully heal.
When can I walk after surgery?
Most surgeons and hospitals today emphasize getting you out of bed quickly. Most people are walking with the assistance of a walker on the day after surgery, and using a cane or nothing at all by two to three weeks.
Can I go directly home after the hospital?Many patients are able to leave the hospital and go directly home after surgery. It is important to identify a family member or friend who will be able to help with common household tasks such as preparing meals and doing dishes. Some patients will require a further stay at a rehabilitation facility.
Will I be able to climb stairs?
In general, patients are able to climb stairs after leaving the hospital; however, it is often initially slow and tiring. This soon improves, but most patients are happiest if initially they are able to stay on one floor after returning home from surgery.
Will I have to take pain medication?
Many efforts are ongoing to reduce the pain patients have after surgery; however, most patients often still do require some pain medications for the first few months after surgery.
Will I need physiotherapy, and if so, for how long?
Most people who have had a total knee replacement require outpatient physiotherapy following surgery. A skilled therapist can accelerate the rehabilitation as well as make the process more efficient with the use of dedicated machines and therapeutic modalities. Depending on your condition before surgery, physiotherapy is beneficial for up to three months and rarely longer. The amount of therapy needed depends upon your condition before surgery, motivation, and general health.
When can I drive?
Most surgeons allow patients to drive at four to six weeks after surgery, and sometimes sooner if the operative leg is the left leg. There is some literature that states that your reaction time will not be back to normal prior to six weeks. You should not drive while on narcotics, and should discuss returning to driving with your surgeon.
When can I return to work?
Returning to work is highly dependent on your general health, activity level and demands of your job. If you have a sedentary job, such as computer work, you may be able to return to work in four to six weeks. If you have a more demanding job that requires lifting, walking, or travel, you may need up to three months for full recovery
What restrictions will I have after surgery?
Restrictions following total knee replacement surgery are generally few and should be discussed with your surgeon. After surgery, you will have some difficulty kneeling on the operative knee, which you will become less aware of with time, but will always have a general perception that the knee is artificial and doesn’t really feel like a normal knee.
Most people are able to return to usual activities and work but may have some difficulty performing heavy labor such as construction or farming. Most sporting activities are fine with the exception of running or jumping.
Traveling should be not be affected by a joint replacement after the first four to six weeks for short trips. Most surgeons advise against prolonged seated travel or flying due to increased risk of blood clot for 12 weeks.
Can I resume sports after a Knee Replacement?
Total knee replacement is a successful procedure in the majority of patients with arthritis. It relieves pain and restores the function and alignment of the joint. If you are considering total knee replacement, you should discuss with your surgeon the possibility of participating in physical activities such as sports following surgery.
Older patients undergoing knee replacement surgery today are more active than in the past, and the surgery is being performed in younger, more active patients. Education and marketing material for patients often depict them enjoying a physically active life after surgery. These factors lead to the question: Can I resume my active lifestyle after knee replacement?
Total knee replacement involves a mechanical device, and the forces applied to the implant are much higher while playing sports than during regular daily activities. These forces could cause wear and tear on the implants. They could loosen, and osteolysis could occur where the bone wears away around the implant as parts of it break down.
Even though implant design and materials have improved over the last 40 years, and surgeons have a better understanding on how the knee replacement responds to the stresses imposed by athletic activities, you should discuss these concerns with your surgeon.
There has not been a major study answering how long knee replacements last in patients who are physically active in relation to those who live a more sedentary life. Surgeons traditionally make recommendations about participation in sports after surgery based on personal preference and “common sense.” The American Association of Hip and Knee Surgeons has these recommendations. Know your body and have realistic expectations.
Having knee replacement surgery doesn’t mean you can participate in strenuous sports that you didn’t do before surgery. The sports you are likely to participate in after surgery are those you played prior to surgery.
Jason C. Ho, MD and co-authors studied 40 patients who underwent total knee replacement surgery. Seventy-five percent of patients participated in high-impact sports before surgery. Ninety-three percent of those patients were able to return to practicing these types of sports after surgery.
Your ability to return to playing sports will also be affected by your general health. Studies show that the healthier you are, the more likely you are to return to playing sports after surgery. Studies also show that if you participated in high-impact sports before surgery, you will be more likely to return to medium and low-impact sports after surgery.
Use common sense.
The greater the impact from playing sports has on your knee implants, the greater chance there may be of damage. You can make the analogy to the tires of your car – the more off-roading you do, the more your tires will wear out.
Stay active after knee replacement!
The beneficial effects of physical activity on your general health and wellbeing are undeniable. With athletic activity, expect better cardiovascular health, muscular strength, endurance, balance, coordination and personal satisfaction.
Which sports are OK?
Remember that physical activities and sports that your surgeon recommends should be performed in moderation. If in doubt, be cautious and protective of your knee replacement!
Low-Impact Sports
Members of The Knee Society recommend that if you’ve had total knee replacement, practicing low-impact activities and sports is fine.
Intermediate-Impact Sports
Intermediate-impact sports are recommended if you have prior experience, but shouldn’t be taken up if you haven’t tried them before.
High-Impact Sports
The majority of doctors do not recommend participating in high-impact sports if you’ve had knee replacement surgery.
Remember that physical activities and sports that your surgeon recommends should be performed in moderation. If in doubt, be cautious and protective of your knee replacement!
Talk to your doctor
It’s important to set expectations with your surgeon prior to surgery to discuss what level of activity is best for you. Ask how long your knee replacement will last if you are very active. Talk about your activities and your involvement in sports. How long your implant tolerates your activities depends on the type of sport you do and how often you do it after surgery. Follow-up exams and x-rays of your knee replacement are necessary to make sure that it continues to function well for a long time.
Risks and complications
Are there complications to total knee replacement surgery?
- Total knee replacement surgery is primarily a pain relieving procedure; however, it may not relieve all pain, and there is a possibility of some residual stiffness and swelling.
- Although complications are relatively rare (1-2% of patients), patients may experience a complication in the postoperative period. These include very serious and possibly life threatening complications such as heart attack, stroke, pulmonary embolism and kidney failure.
- Stiffness or loss of motion can also occur.
- Infection (1%) is one of the most debilitating complications and often requires prolonged antibiotics with several additional surgeries to rid the infection.
- A blood clot in the leg is also a relatively common complication requiring some type of blood thinner following surgery to reduce the incidence.
- The implants can also fail over time due to wear or loosening of the components, but this generally occurs many years after surgery.
- Patients who are overweight, smoke, have liver or kidney disease and have diabetes are at higher risk of complications following surgery.
- Patients with depression, anxiety, chronic pain conditions (such as lower back pain) are prone to having less improvement and satisfaction following knee replacements